Stem cell research is surrounded by loaded controversy over the bioethical issues that it poses.
What many people don’t understand is that there are two different types of stem cells currently being used for research: embryonic and adult. Adult stem cell use is not the cause for discussion, allowing research to continue with the hopes of changing the treatment of disease.
Researchers worldwide, who have already developed various therapies to treat leukemia, also hope to treat cancer, Parkinson’s disease and spinal cord injuries one day. Now, Boston-based researchers have made the next development in stem cell studies, which will reap exciting benefits for a large population of patients suffering from inflammatory diseases.
A group of researchers from Brigham and Women’s Hospital, the Harvard Stem Cell Institute, Massachusetts Institute of Technology and Massachusetts General Hospital have uncovered a way for stem cells to act as a ‘drug factory’ at the site of inflammation in the body, according to a study published Oct. 4 on EurekAlert.
Oren Levy, the head researcher, said he is optimistic about the discovery’s potential to treat diseases such as myocardial infarction, multiple sclerosis and even certain types of cancer.
“It’s important not to create false hope, but we do see a lot of progress to be made,” Levy said.
What did they do?
Levy, with the help of collaborators Jeffrey Karp, Weian Zhao, Mehmet
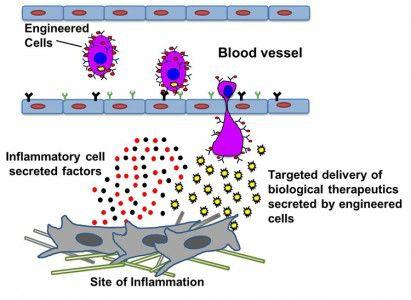
Modified strands of mRNA were inserted into connective tissue stem cells called mesenchymal stem cells (MSC), which are a type of adult stem cells. Upon mRNA insertion, the cells produced an anti-inflammatory molecule known as interleukin-10.
These modified human stem cells were then injected into the bloodstream of a mouse that was experiencing inflammation in the ear. The cells targeted the site of inflammation and released the anti-inflammatory
“We basically used the cells as a vehicle to deliver, and they did,” Levy said.
He said the cells effectively delivered the molecule and successfully suppressed inflammation.
Mariah Cassum, a senior in the Sargent College of Health and Rehabilitation Sciences, said she wonders how safe the MSC manipulation is.
“After looking at the study, I’m concerned with the fact that the normal MSC immunomodulatory properties are highly variable and uncertain,” she said. “What are the potential risks of manipulating such a naturally unstable cell?”
Researchers are using MSCs more frequently because of their ability to evade the immune system. Even when derived from another person, MSCs are still safe to use elsewhere.
However, the use of MSCs still poses several challenges. They have a “hit-and-run” effect, meaning that they are cleared rapidly after entering the bloodstream. Despite this possibility, the research group managed to see a therapeutic effect on the inflamed tissue in the mouse, meaning the site of inflammation was eliminated.
Levy said he and the researchers plan to test ways to prolong the cells’ lifespans and to ensure the best treatment.
The modification of the mRNA came from a technique developed by Yanik in his MIT lab. This programming does not alter the cell’s genome, making the process harmless.
What does it mean?
In a statement from the Harvard Stem Cell Institute, Karp summarized the study’s findings.
“If you think of a cell as a drug factory, what we’re doing is targeting cell-based, drug factories to damaged or diseased tissues, where the cells can produce drugs at high enough levels to have a therapeutic effect,” he said.
Ultimately, the group was able to develop a type of cell that has the capability of reaching the site of inflammation to suppress the disease.
As one of the first successful studies to target a disease site with biological drugs, biopharmaceutical companies are paying close attention to the work of Levy and his colleagues. Although biological drugs can be highly effective alternatives to regular pharmeceuticals, Levy said they still pose challenges for use. The lifespan of the cells, the ability to target the correct area of the body and finding the correct drug to treat the correct patient are just a few of the potential issues that physicians and researchers face.
Aside from these impending complications, the study proved that clinical applications may be possible.
“If you think about biological therapeutic drugs, they’re a huge part of medicine, but there’s still challenges,” Levy said. “It’s hard to target them where you want them to act.”
Though this study looked at a simple local inflammation model in the ear of a mouse, the group was able to target the specific site of inflammation, which they said will have larger implications in the medical field.
Levy said the research group hopes to develop a clinically relevant model in the future. However, he noted the research “has a lot of potential happening in the next few years to come, but it’s still early.”
The future of these ‘drug factories’
Chronic inflammation can lead to diseases such as atherosclerosis, arthritis and even some cancers. The research the group garnered can potentially treat, and perhaps one day eliminate, some of these diseases.
“I’m interested in seeing how this research develops and becomes incorporated into our methods of treating inflammation,” Cassum said. “Stem cell treatment could be the future of drug therapy.”
After testing the ability of the cells to make their way to the site of inflammation, their methods were successful.
“We were able to get cells where we wanted them to go and we could make cells secrete high levels at the site,” Levy said. “Many tragic diseases are inflammatory and we could help those.”
Queena Liang, a senior in SAR, said she believes this development could potentially aid in the treatment of disease and tragic accidents.
“It will be useful in hospitals with patients who have large-scale inflammation and trauma issues,” she said. “Your body’s defense mechanism when you get into a car crash is to respond with inflammation, so maybe this could help patients in that situation.”
Although the steps toward treating larger-scale diseases with this therapy will only come with time and additional progress in the lab, Levy said he and his colleagues are optimistic about the research’s future.
“We’re interested to explore the platform nature of this approach and see what potential limitations it may have or how far we can actually push it,” Zhao said in a public statement.
Levy is building his research off of other scientific cell studies and progress in the science field as well.
“We’re harvesting the knowledge that we already have to hopefully modify cells to go to any relevant organ that needs treating,” Levy said. “We see a lot of progress for autoimmune diseases and other inflammatory diseases.”
Julia Brandeis, a senior in SAR said, “It’s great that there’s advancements in medicine, and hopefully this will be beneficial for the search to cure diseases that many people suffer from.”
Though there is still a lot to come from stem cell research, Levy and his group have made progress and headway in the race for an efficient treatment.
“We’ll keep on trying and keep on optimizing the process until we get a maximal response,” he says. “We’ll keep an open mind until we solve it.”